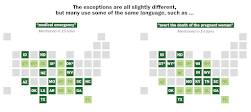
1. Abortion. The Texas Tribune has a good story on the history of this litigation and Tuesday's ruling (State of Texas et al. v. Becerra, No. 23-10246 (Jan. 2, 2024). The court upheld a permanent injunction against an HHS injunction against DHHS's post-Dobbs guidance that the Emergency Medicine & Active Labor Act (EMTALA) requires Medicare providers to perform an abortion when that is necessary to stabilize a pregnant woman's emergency (life- or limb-threatening) condition. The court concluded that Congress did not intend for the statute to require performance of a procedure that was forbidden by state law. The court went on, asserting that Texas law provides plenty of protection for procedures, including abortion, when continuing the pregnancy poses a threat to the pregnant woman's life or a major bodily function. This is the same line taken by the Texas Supreme Court in its opinion that denied Kate Cox's bid for an abortion under the same exception to the state's abortion ban.
Meanwhile, according to Kate Riga at TalkingPointsMemo.com, the same issue is in front of the 9th Circuit Court of Appeals. Depending on the outcome of that case, the issue may land at SCOTUS's doorstep soon.
2. E-cigarettes. The case is Wages and White Lion Investments, L.L.C. v. Food & Drug Administration, No. 21-60766 (Jan. 3, 2024). This was an en banc proceeding of the Court of Appeals, with a majority opinion by Judge Oldham (and joined by nine others) and a dissenting opinion by Judge Haynes (joined by four others). The result of the case is that the FDA is ordered to review over 1 million pre-market tobacco applications (PMTAs) against the backdrop of clear and convincing evidence that e-cigs represent a serious health threat, especially to minors, with no countervailing health benefits.
This is Judge Haynes' take on the majority opinion (emphasis added):
It is against this backdrop that the FDA reviewed the PMTAs of Wages and White Lion Investments, LLC, d/b/a Triton Distribution (“Triton”) and Vapetasia LLC (“Vapetasia”) (collectively, “Petitioners”) and issued marketing denial orders (“MDOs”) to Petitioners. The FDA denied Petitioners’ PMTAs because they did not contain any reliable evidence suggesting the benefits of Petitioners’ flavored products outweighed the significant risks to youth—an outcome that aligned with both the guidance the FDA had given to applicants and its statutory mandate under the TCA. But the majority opinion erroneously concludes that the FDA changed the evidentiary standards applied to Petitioners’ PMTAs and wholly ignored Petitioners’ marketing plans, and thus acted in an arbitrary and capricious manner. Unfortunately, based on a misreading of the law and a misconstruing of the relevant facts, the majority opinion supersedes the FDA’s work by remanding instead of denying the petition, which cuts the FDA’s legs out from under it in the middle of a dangerous and constantly evolving public health crisis.
In so doing, the majority opinion also departs from all but one of our sister circuits that have addressed the same issue. See, e.g., Magellan Tech., Inc. v. FDA, 70 F.4th 622 (2d Cir. 2023) (unanimous denial); Liquid Labs LLC v. FDA, 52 F.4th 533 (3rd Cir. 2022) (unanimous denial); Avail Vapor, LLC v. FDA, 55 F.4th 409 (4th Cir. 2022) (unanimous denial), cert. denied, No. 22-1112, 2023 WL 6558399 (U.S. Oct. 10, 2023); Gripum, LLC v. FDA, 47 F.4th 553 (7th Cir. 2022) (unanimous denial), cert. denied, 143 S. Ct. 2458 (2023); Lotus Vaping Techs., LLC v. FDA, 73 F.4th 657 (9th Cir. 2023) (unanimous denial); Prohibition Juice, 45 F.4th 8 (unanimous denial); see also Breeze Smoke, LLC v. FDA, 18 F.4th 499 (6th Cir. 2021) (denying motion for stay), app. for stay denied, 142 S. Ct. 638 (2021). The only circuit that granted a petition for review in a comparable context did so on much narrower grounds than the majority opinion embraces today. See Bidi Vapor, 47 F.4th at 1195 (remanding based on the FDA’s failure to consider marketing and sales-access-restriction plans); but see id. at 1208–18 (Rosenbaum, J., dissenting). Despite the Eleventh Circuit’s opinion, however, it is telling that the Supreme Court recently denied certiorari for two cases in which other circuits considered similar facts to those before us and denied the petition for review. See Gripum, LLC v. FDA, 143 S. Ct. 2458 (2023) (mem.); Avail Vapor, LLC v. FDA, No. 22-1112, 2023 WL 6558399 (U.S. Oct. 10, 2023) (mem.); see also Breeze Smoke, LLC v. FDA, 142 S. Ct. 638 (2021) (mem.) (denying application for stay of FDA’s denial, without any recorded dissent).
Reevaluating this case en banc, I would reach the same determination that the merits panel did and deny the petitions for review before us.
I concur.